How to Test Cortisol Levels: Methods, Timing, and Next Steps
Someone tells you your cortisol might be off. Or you’ve been reading about fatigue, unexplained weight gain, and sleep that never feels restorative — and you keep seeing the same word come up: cortisol. So you look up how to test cortisol levels, and suddenly you’re staring at three different testing options with no clear guidance on which one applies to you, when to take it, or what the number will actually mean.
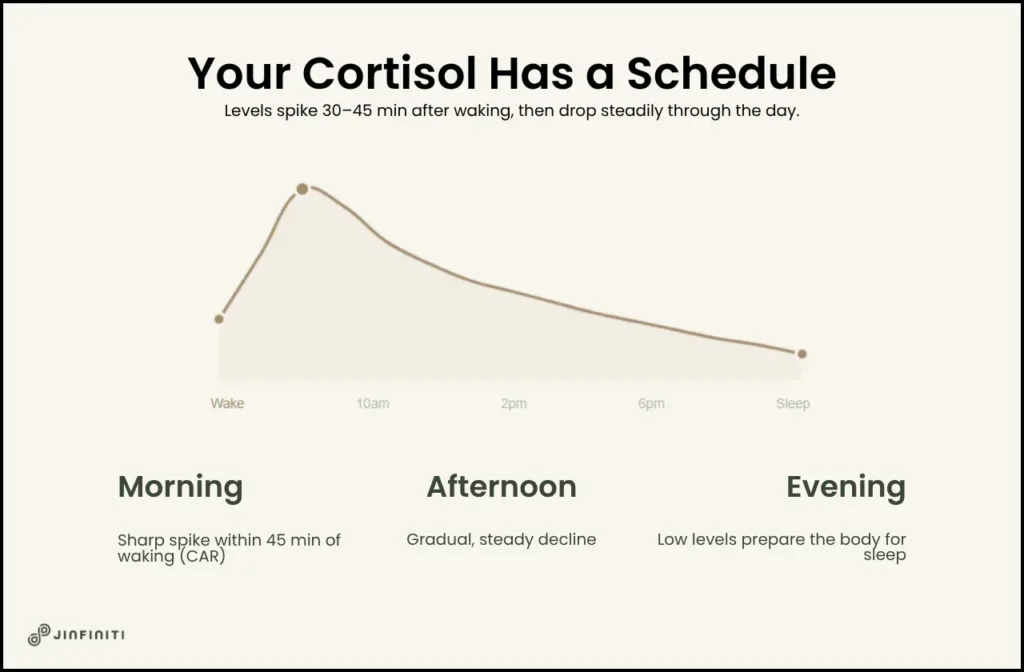
Here’s the thing that makes cortisol testing confusing: cortisol isn’t a fixed number. It follows a predictable daily arc — rising sharply in the morning, declining through the day, bottoming out at night. The type of test you use, when you collect the sample, and how you prepare will determine whether the result tells you something meaningful. A single morning blood draw and a four-point salivary panel are measuring very different things.
This guide breaks down each method, explains why timing matters more than most articles acknowledge, and covers what to do — and what to look further into — once you have your results.
What You Should Know
- Cortisol follows a daily rhythm, so the best test depends on which part of that rhythm you’re trying to assess.
- Salivary cortisol testing is the most practical at-home option and captures the full daily pattern, not just a snapshot.
- A “normal” cortisol result doesn’t always explain persistent fatigue — cortisol measures stress physiology, not cellular energy status.
CLIA-Certified NAD Test Kit
Cortisol doesn’t tell the whole story.

Why Cortisol Levels Change Throughout the Day
Understanding why cortisol moves the way it does is what makes cortisol testing interpretable. Without that context, a result is just a number.
Cortisol is produced by the adrenal glands and regulated by the hypothalamic-pituitary-adrenal (HPA) axis — a feedback loop connecting the brain to the adrenal glands. The HPA axis responds to signals from the body’s internal clock, stress inputs, blood sugar, and immune activity. Cortisol’s job is to mobilize energy, sharpen alertness, and prepare the body for demands ahead. It does that job on a schedule.
The Cortisol Awakening Response
Within the first 30 to 45 minutes after waking, cortisol levels spike — sometimes doubling from overnight lows. This is the cortisol awakening response (CAR), and it’s one of the more reliable windows into how well the HPA axis is functioning. A robust morning rise is associated with better alertness, immune regulation, and metabolic stability across the day. A blunted one — where the morning spike is flat or minimal — shows up frequently in people dealing with burnout, prolonged fatigue, and low-grade chronic stress.
After the morning peak, cortisol follows a gradual decline. By evening, levels should be low enough to allow the body to wind down and sleep.
What a Disrupted Pattern Looks Like
Under chronic stress, that arc gets distorted. Cortisol may stay elevated longer than it should, or — after sustained overactivation — the system exhausts itself and levels flatten out entirely. Neither pattern shows up clearly in a single morning blood draw. You’d see a number that looks broadly normal at the wrong moment, with no picture of how the hormone behaves across the full day.
This is why multi-point testing is considered more informative for evaluating everyday HPA function. One number in isolation doesn’t tell you much about rhythm — which is the part that actually affects how you feel.
The Three Main Ways to Test Cortisol Levels
Each testing method measures something slightly different. Matching the method to your goal matters more than most people realize.
Salivary Cortisol Testing
Salivary testing is the most practical way to check cortisol levels at home, and it has solid clinical backing. It measures free cortisol — the biologically active form — rather than total cortisol, which includes the portion bound to proteins and not available to act on tissues. Research in Nature Clinical Practice Endocrinology & Metabolism has validated salivary cortisol measurement as a clinically accurate approach, particularly for capturing cortisol at its daily nadir and assessing the morning pattern.[1]
For at-home use, comprehensive kits typically ask for four samples: immediately upon waking, around noon, late afternoon, and before bed. This multi-point approach gives a picture of the full daily arc. You can see whether the morning response is adequate, whether cortisol is declining appropriately through the day, and whether evening levels are low enough to support good sleep. That’s a lot more information than a single data point.
Blood Cortisol Testing
Blood testing is the standard clinical approach, typically drawn between 7 and 9 a.m. — the expected peak — to produce a standardized, comparable result. As MedlinePlus notes, draws are sometimes repeated later in the day to assess whether cortisol is following the expected decline, but single-time-point morning draws are far more common in routine clinical care.
Blood tests measure total cortisol, which includes both the free and protein-bound portions. For adrenal disorder screening — Cushing’s syndrome (excess production) or Addison’s disease (insufficient production) — it’s the standard method. For assessing everyday HPA function and stress-related cortisol disruption, the picture is less complete.
24-Hour Urine Testing
A 24-hour urine collection captures everything the body excretes over a full day, giving a comprehensive measure of total cortisol output rather than a moment-in-time value. This method is more common in clinical settings where there’s reason to evaluate overall adrenal production — particularly when ruling out Cushing’s syndrome or other cortisol-excess conditions.
It’s less useful for identifying a disrupted daily rhythm, since it averages everything across the full day. But for questions about total cortisol load, it provides reliable data that snapshot tests can’t.
How to Prepare for an Accurate Cortisol Test
Cortisol is responsive — to exercise, stress, sleep quality, food, and several medications. Getting a result that reflects your actual baseline means controlling for as many of those variables as possible.
A few things to account for before testing:
- Exercise: Intense physical activity raises cortisol acutely. Most clinicians recommend avoiding strenuous workouts in the 24 hours before testing.
- Medications: Corticosteroids (including topical skin creams), hormonal birth control, and high-dose biotin supplements can all affect readings. Don’t stop any prescribed medication without talking to your clinician first — just make sure they know what you’re taking when they interpret results.
- Stress and sleep: Testing during an unusually difficult week, after significant sleep disruption, or following a stressful event is more likely to capture an outlier than your actual pattern.
- For saliva samples: Don’t eat, drink (anything other than water), brush your teeth, or smoke for at least 30 minutes before collecting. For morning samples, collect within minutes of waking — before getting up, making coffee, or reaching for your phone.
Testing on a day that reasonably represents your normal — not your worst week, not your best — produces results worth interpreting.
How to Read Your Cortisol Results
Reference ranges vary by method and lab, so a number should always be read against the context provided by your testing kit or clinician rather than a generic threshold. For morning serum cortisol in adults, typical ranges fall between roughly 6 and 23 mcg/dL, though this varies by assay. Afternoon values are expected to be meaningfully lower than morning values.
For salivary testing, the pattern matters as much as any individual value. A healthy arc shows a clear morning peak, a gradual decline through the day, and low evening levels. What to look for in disrupted patterns:
- Flat curve (morning and evening values close together): Suggests HPA dysregulation, often associated with burnout or prolonged stress.
- Consistently elevated values: May warrant further clinical evaluation for cortisol excess.
- Very low values throughout: Can indicate adrenal insufficiency, particularly when paired with symptoms like fatigue, dizziness, or salt cravings — worth discussing with an endocrinologist.
It’s worth saying clearly: abnormal cortisol results don’t diagnose a condition on their own. Disrupted patterns are common in people managing chronic stress, sleep disorders, and burnout — without any underlying adrenal disease. Results should be interpreted in context, and any follow-up testing or treatment decisions should involve a clinician.
When Cortisol Testing Isn’t the Whole Picture
Here’s a situation that comes up often: someone tests their cortisol, the results look broadly normal, and they’re still exhausted. Still foggy. Still not recovering the way they used to. If that sounds familiar, the issue usually isn’t that the test was wrong — it’s that cortisol measures stress system activity, not what that stress has done to the cells downstream.
Research published in Physical Therapy describes how prolonged HPA activation — the kind that accumulates over months or years of sustained stress — can lead to cortisol dysfunction and widespread inflammation that persists even after stress levels normalize. The signaling system gets dysregulated.[2]
And separately, research published in Molecular Neurobiology found (in animal models) that psychological stress reduced mitochondrial respiration in the prefrontal cortex by up to 50%, effectively cutting cellular energy output in half. That downstream effect — depleted cellular energy at the mitochondrial level — isn’t something cortisol testing measures.[3]
NAD+ (nicotinamide adenine dinucleotide), the molecule that sits at the center of cellular energy production, declines under sustained oxidative and inflammatory stress. And unlike cortisol, which may normalize while fatigue continues, intracellular NAD+ levels reflect what’s happening inside the cell right now. For people whose fatigue doesn’t resolve despite normal test results, that distinction matters.
As Dr. Jin-Xiong She, founder of Jinfiniti Precision Medicine, explains: “Cortisol tells you that the stress response has been activated. What it doesn’t tell you is what that stress has cost your cells. That’s where NAD+ measurement becomes important — you can’t address cellular energy depletion without first measuring it.”
What to Do After Getting Your Results
If results are significantly outside the expected range, follow up with a clinician — ideally an endocrinologist if an adrenal condition is suspected. Cortisol testing alone can’t identify the cause of an abnormal result; further workup is typically needed.
If results look broadly normal but symptoms persist, treat that as information too. It tells you the problem is probably not a primary adrenal disorder, and shifts the investigation toward other systems: sleep architecture, thyroid function, metabolic health, and cellular energy production are all reasonable next areas depending on your specific picture.
Whatever direction you go, measuring before making changes — rather than starting cortisol-lowering supplements or protocols based on symptoms alone — tends to produce better outcomes. That applies to cortisol and to everything downstream of it.
Frequently Asked Questions
What is the best time of day to test cortisol levels?
For blood tests, between 7 and 9 a.m. captures the expected morning peak. For salivary testing, the most informative approach is a four-point collection: at waking, around noon, late afternoon, and before bed. Multi-point salivary testing gives a picture of the daily arc that a single morning draw can’t.
Can I test cortisol levels at home without a doctor?
Yes. CLIA-certified at-home salivary cortisol kits are available without a prescription and can provide a clinically valid picture of your cortisol rhythm. Abnormal results — or normal results that don’t explain your symptoms — are worth discussing with a clinician for proper interpretation and follow-up.
How accurate are at-home salivary cortisol tests?
Salivary cortisol is a clinically validated method for measuring free cortisol. Accuracy depends heavily on following collection instructions precisely: timing, prep steps, and testing on a representative day all affect the result. Kits from accredited labs with proper certification tend to perform reliably when used correctly.
What cortisol level is considered normal?
For morning serum cortisol, typical adult reference ranges are approximately 6–23 mcg/dL, though this varies by lab. For salivary tests, ranges differ by assay and time of day. A single number without timing context is hard to interpret — the expected range for 8 a.m. is very different from the expected range for 10 p.m.
What does a flat cortisol curve mean?
A flat curve — where morning and evening values are similar rather than separated by a clear peak-to-trough decline — suggests HPA axis dysregulation. It’s commonly associated with burnout, prolonged fatigue, and chronic stress. It’s worth discussing with a clinician, especially when paired with symptoms that don’t have another clear explanation.
Can low NAD+ levels cause the same symptoms as high cortisol?
They can overlap considerably. Both are associated with fatigue, cognitive sluggishness, disrupted sleep, and reduced recovery capacity. They often occur together — prolonged cortisol dysregulation contributes to oxidative stress and NAD+ depletion over time. Measuring both, rather than assuming one explains the other, gives a more complete diagnostic picture.